By James Troup
Data will now and forever play a major role in the relationships between patients, insurers and healthcare providers. If your organization doesn’t get on board early, you could be left behind. Driving the lion’s share of the data collection requirements is the HITECH (Health Information Technology for Economic and Clinical Health Act) through the demonstration of Meaningful Use (MU), as well as pilot ACO’s (Accountable Care Organizations), PCMH (Patient Center Medical Home) and pay-for-performance ( P4P) ; all requiring data governance, standards, and quality assurance. Soon, if not already, you’ll be sharing this data through an HIE (health information exchange) to other providers, and a patient portal where your patients will have access to their records. In any event, data governance will play a large role in your ability to operate effectively.
Although the technology is simply “1” and “0”, the information is PHI (protected heath information), and that makes the collection, storage, and analysis complicated- and there is a lot of it. Just to get your head around the amount of data being stored, an estimate of Pediatric Alliances’ database, with 50,000 active patients has approximately 500 gigabytes (GB) of data. At 50,000 patients/500 GB, equals approximately 10 megabytes (MB) per patient- and growing at 50 GB per year at $3.00 per GB. Let me break it down into everyday life; a GB is about 250 songs on your iPod, and a MB is the equivalent of a 500 page book. So healthcare, an industry that has the proclivity to have nominal standards in regard to data collection is now leveraging “Big Data”.
Big Data, defined by Gartner, a leading technology research and advisory firm, as the volume, velocity, variety, or complexity of information. This is all part of the new world of healthcare that has moved into the business of data warehousing. But when we start to share this data, to improve clinical outcomes, the problems lie in the wide variation in information technology adoption and capabilities across physician practices, particularly by physician practice size. There are over 800,000 physicians in America. (AMA 2009). Working towards a standard to exchange, measure, analyze and report on clinical data across the sea of providers seems daunting, if not impossible at first. If every heath system does it part by managing to standards, and putting in place a data governance process, then we’re well on our way to having a national health information exchange- where health information will follow consumers, is available for providers for clinical decision making, and improves the overall population health.
How can your organization be part of the solution and develop a data governance plan?:
- Put together a cross-functional team- Thinking through the strategy and the value added to the organization by the group participants will promote buy-in. Teams will vary in size and discipline, but a broad perspective will provide the most impact. One caveat is not to overdo it with the number of team members, but make sure there is representation.
- Establish a framework-A strong data governance program h
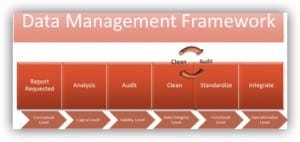
 as a framework that drives value into the business by defining the methods used to establish quality. Below is an example of a framework that I deployed to manage quality in the requesting and reporting on data. There are six levels of analysis that following a six-step process on all reports that are published in the enterprise:
as a framework that drives value into the business by defining the methods used to establish quality. Below is an example of a framework that I deployed to manage quality in the requesting and reporting on data. There are six levels of analysis that following a six-step process on all reports that are published in the enterprise:
- Report Request (Conceptual Level): A request form was standardized and used to manage and archive requests from management and providers. The request form accompanies all reports and acts as a change request control document for updating, editing or monitoring report performance.
- Analysis (Logical Level): A review of the report request form is sent to the data governance team for review. This allows for feedback on the design and how the request works procedurally by clearly defining the requirements of the report.
- Audit (Validity Level): Once the report was designed a test was administered by sampling the data. The report was sent to the data governance team and tested for face validity, and reliability by recreating the episode or event to be reported on.
- Clean (Data Integrity): Once the report was tested the results were either entered into a cyclical auditing process until the standard was meeting or standardized into the functional level.
- Standardized (Functional Level): At the functional level, the reports have now met the required standard, and the data management team establishes procedures for utilizing the report.
- Integrate (Operational Level): At the operational level, the end users are trained on how to administer the report, and the data management team continues to monitor the desired outcomes. All audits or changes are sent through the process as a change request through the report request form.
- Pilot- Building slowly and looking for low hanging fruits build momentum for the team and also demonstrate the value to the organization. So, try a pilot on a sample data point that is valuable. I started our program by capturing an email address. I was able to demonstrate the value immediately. I would also suggest that the pilot offer you the ability to:
- Reflect on lessons learned.
- Refine your process and look for improvements.
- Report back to stakeholder on the progress made.
4. Operationalize– Begin to address quality by aligning activities with strategic initiatives. Some suggestions, obvious I’m sure, MU, ACO contracts, PCMH initiatives and P4P.
As much as data governance is important to the future of our healthcare system, there are other data challenges. Understanding that data come in two forms, structured and unstructured, the focus of the suggestions above are based on structured data. Structured data is a set of organized fields and can easily be reported on, while unstructured data continues to elude us and is everything else It’s estimated that 60 percent of healthcare data resides outside of health information systems in unstructured documents limiting our ability to fully understand and evaluate the entire 10 plus MB per patient record. A solution is down the road and tagging a document for now can provide some relief for retrieval. Maybe OCR (optical character recognition) will provide the solution- stay tuned.
About the Author
James Troup, M.S. MIT, currently serves as the Chief Executive Officer of Pediatric Alliance. He has twelve years of senior management experience with a major focus on technology, and business strategic planning and alignment. He is an active member of HIMSS, PAeHI, MGMA, ACHE, and the Project Management Institute. James holds a Master’s of Science in Management and Information Technology from the University of Virginia.
About Pediatric Alliance
Formed in 1996, Pediatric Alliance has grown to be the largest physician-owned group pediatric practice in Southwestern Pennsylvania. Pediatric Alliance is devoted to providing high-quality, comprehensive primary car to infants, children and adolescents through clinical expertise, advocacy, education, collaboration, research and information management.