
Key for Costliest Health Plan Members and Employee Claimants
By Pam Greenhouse
The total cost of chronic disease in American between 2016-2030 is projected to be $42 trillion, according to the Partnership to Fight Chronic Disease, with $8,600 per person in medical and productivity cost if current trends continue.
The U.S. Department of Health and Human Services Agency for Healthcare Research and Quality reports that over half of Americans are living with at least one chronic condition and nearly a third have multiple chronic conditions including congestive heart failure, diabetes, arthritis, and depression. Individuals with multiple chronic conditions are also the costliest patients, and costs increase with the number of chronic conditions: In 2010, nearly 40% of all inpatient hospital stays were for those with 5+ chronic conditions.
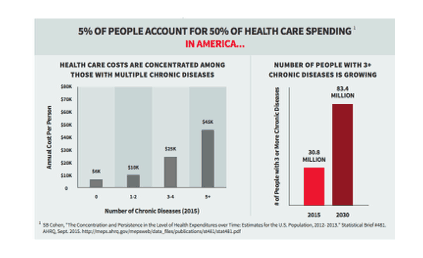
While these costs have skyrocketed for decades unabated, we have reached a tipping point where the evolution of mobile technology combined with video health coaching, such as youtube to mp4 converter, can address both the cost and quality challenges this population presents.
In the late 1990s-early 2000s, disease management programs (DMPs) began to proliferate, driven by managed care and capitation, with the aim of lowering the cost of care for chronic disease. But the challenges of patient enrollment and compliance have been significant and DMPs haven’t reached their potential. In fact, a not-insignificant number of companies have given up on DMPs for these reasons.
Today, mobile technology has evolved; in 2017, there were 3.7 billion health app downloads, according to a leading provider of market and consumer data, Stastista. At the same time, there is growing awareness of, and interest in, health coaching among companies (as a mechanism for lowering cost of care) and individuals (for improving health); a recent Survata poll showed that a majority of individuals are actively interested in receiving health coaching. Yet, on their own, we don’t see health apps or health coaching replacing or supporting DMPs enough to begin to turn around the tremendous cost of chronic disease in the United States.
However, there is a sweet spot where combining mobile technology and professional health coaching in an intentional and systematic way overcomes the challenges of enrollment, compliance, and retention, reduces avoidable hospitalizations and ER visits for chronic disease, and creates a win-win-win – for individuals, for health plans and companies, and for the health economy of the country.
The right combination brings very simple and accessible technology into the hands of those with chronic disease(s) and connects them with health professionals (master’s prepared social workers, nurses, and chronic disease specialists) who can remotely monitor their symptomatology daily in real-time and provide frequent regularly-scheduled education and ongoing coaching toward behavior change through face-to-face video chat. This model creates an augmented level of patient-coach partnership for accountability and retention, and supports the individual’s sense of achievement, confidence, and their understanding of how to seek the right level of care at the right time.
This two-pronged approach of the daily window into symptomatology and the longer engagement involving education, goal-setting, behavior change, and problem-solving offers the opportunity to intervene before disease symptoms require an ER visit or hospitalization, and the opportunity to change habits, lifestyle, and address barriers, all of which can significantly impact the course and progression of chronic disease.
The end-goal of significantly improving individuals’ and patients’ abilities to self-manage chronic disease(s) and to decrease avoidable hospitalizations and ER visits is at hand.
For health plans and for self-insured companies’ high cost claimants, partnering with a company that offers the right combination of technology and human touch in disease management is an excellent return on investment, and improved quality of life and customer experience for their members and employees.
Pamela Greenhouse is the Vice President of Clinical Operations at Wellbridge Health, Inc. Wellbridge Health is a tele-health care management company that offers an innovative care management program designed to address the needs of those with chronic disease(s) that make it difficult to effectively manage their medical costs. Ms. Greenhouse holds an M.B.A. in Organizational Behavior and has co-authored over 30 papers in peer-reviewed scholarly journals with a focus on improving care delivery and patient- and family-centered care. For more information, email Pamela at [email protected].







