Defining the Synergy Between Healthcare and Wellness
Understanding the landscape of well-being begins with a clear distinction between healthcare and wellness, two terms often used interchangeably but representing fundamentally different approaches. Healthcare, traditionally, is a reactive system, primarily focused on diagnosing, treating, and managing illnesses and injuries. It’s the infrastructure of hospitals, clinics, specialists, and pharmaceuticals that intervenes when health issues arise.
Wellness, conversely, is a proactive and holistic pursuit. It’s about making conscious choices and adopting lifestyles that lead to a state of optimal physical, mental, and emotional health. It emphasizes prevention, self-care, and continuous improvement across various dimensions of life. In 2026, the integration of these two concepts is becoming increasingly vital, moving us towards a more comprehensive and sustainable model of well-being.
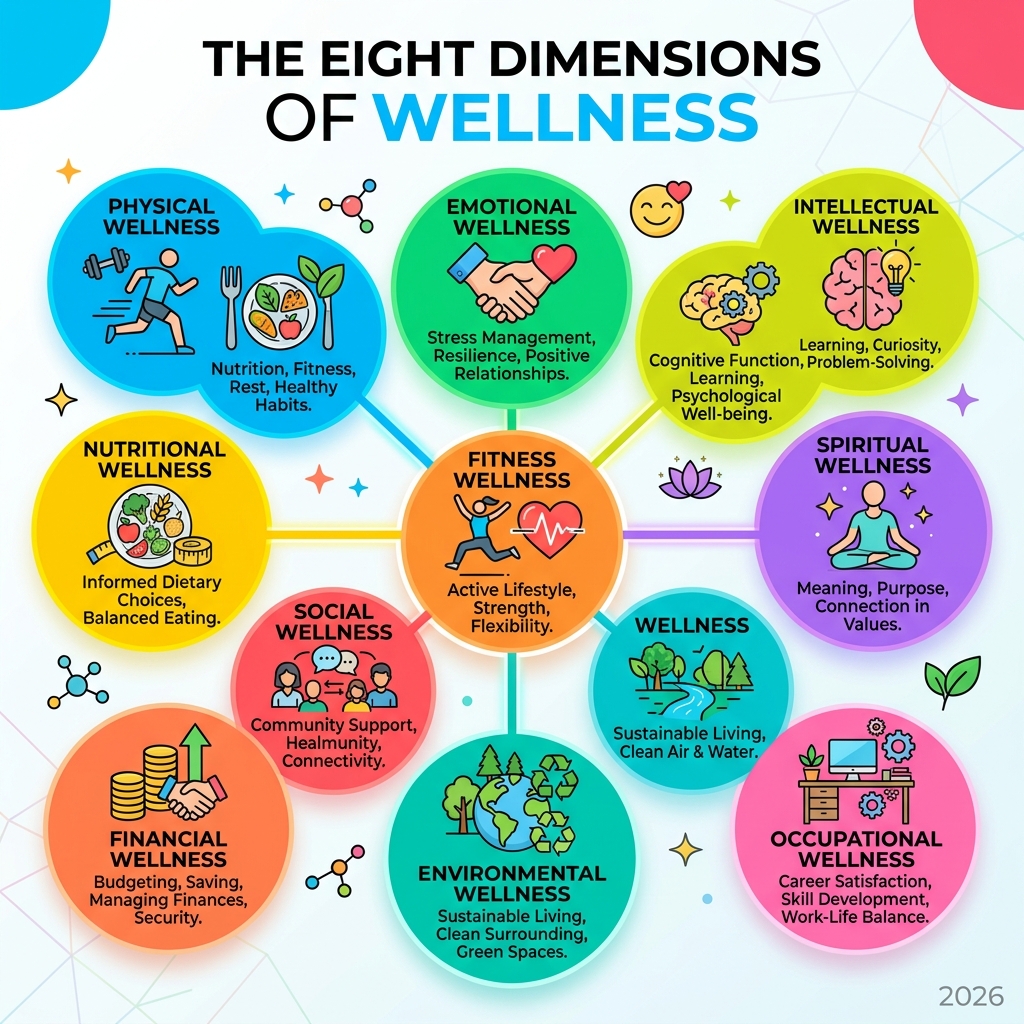
Reactive Healthcare Proactive Wellness Focuses on illness, injury, and disease treatment Focuses on prevention, optimal health, and vitality Intervenes when problems occur Cultivates habits to avoid problems Often episodic and crisis-driven Continuous, lifestyle-driven, and self-directed Primarily medical interventions Encompasses physical, mental, emotional, social, etc. The journey to holistic health involves nurturing several key dimensions. Physical health, for instance, encompasses nutrition, fitness, and adequate rest. Emotional stability involves managing stress, fostering positive relationships, and developing resilience. Mental clarity refers to cognitive function, learning, and psychological well-being. Nutritional foundations are built on balanced eating, understanding food’s impact on our bodies, and making informed dietary choices. Fitness goals drive us to maintain an active lifestyle, improving strength, flexibility, and cardiovascular health. Spiritual wellness, often overlooked, relates to finding purpose, meaning, and connection in life. Environmental factors consider our surroundings and their impact on our health, advocating for clean air, water, and sustainable living. Social connectivity emphasizes the importance of community and supportive relationships, while financial well-being addresses the stress and health impacts of economic stability.
These dimensions are interconnected, and a deficit in one can impact others. This holistic view is why preventive care is so crucial. As highlighted by the Centers for Medicare & Medicaid Services (CMS), Preventive Care aims to block or delay illness, enable early detection, improve health outcomes, and ultimately reduce costs. Over half of all adult Americans live with at least one chronic disease, such as heart disease, cancer, and diabetes, which are the leading causes of death and disability. Proactive wellness, supported by preventive healthcare, empowers individuals to manage their health proactively, rather than waiting for symptoms to emerge.
Digital Tools for Healthcare and Wellness
In April 2026, digital literacy plays a pivotal role in empowering individuals to manage their health and wellness. The proliferation of digital tools has transformed how we access information, track progress, and engage with our personal health journeys. Self-care apps, for example, offer guided meditations, sleep tracking, and mood journaling, providing accessible support for emotional and mental well-being. These tools help individuals build consistent habits and foster greater self-awareness.
Symptom checkers, often backed by extensive medical databases, offer preliminary insights into potential health concerns, guiding users on whether to seek professional medical advice. While not a substitute for a doctor’s diagnosis, they serve as valuable first-line resources. Health encyclopedias, like those found on WebMD – Better information. Better health., provide comprehensive, medically reviewed information on thousands of conditions, treatments, and healthy living topics. WebMD, a leader in digital health publishing for over 25 years, reaches over 50 million monthly readers with content reviewed by 130 medical experts.
Wearable tracking devices have become ubiquitous, monitoring everything from heart rate and sleep patterns to activity levels and stress indicators. This real-time data empowers individuals to make informed lifestyle adjustments and share pertinent information with their healthcare providers. Telehealth integration, accelerated in recent years, continues to expand, offering virtual consultations, remote monitoring, and digital prescriptions, making healthcare more convenient and accessible than ever before. These digital advancements are not just about convenience; they are about fostering a more informed, engaged, and proactive approach to personal health management.
Socioeconomic Access to Healthcare and Wellness
Access to quality healthcare and wellness resources remains a significant global challenge, varying dramatically based on location, insurance status, and socioeconomic factors. Geographic barriers can limit access for those in rural or underserved areas, where specialists and advanced medical facilities may be scarce. In contrast, urban centers often boast a higher concentration of diverse healthcare providers and wellness opportunities.
Insurance coverage is another critical determinant. In systems where private insurance plays a dominant role, such as the United States, individuals without adequate coverage may face prohibitive costs, leading to delayed care or avoidance of necessary treatments. Publicly funded systems, common in many other developed nations, aim to provide universal access, though they can face challenges related to funding, wait times, and resource allocation. The Wikipedia article on Health care provides a comprehensive overview of how health systems worldwide are structured and financed. For instance, the US healthcare industry accounted for 18% of its gross domestic product in 2020, significantly higher than many other nations. Despite this spending, access and outcomes can still be disparate.
Health literacy, the ability to understand and use health information, also plays a crucial role. Individuals with lower health literacy may struggle to navigate complex healthcare systems, understand preventive guidelines, or make informed decisions about their well-being. Socioeconomic disparities, including income, education, and employment, profoundly impact health outcomes. These factors influence everything from access to nutritious food and safe living environments to the ability to afford co-pays or take time off work for appointments. In 2026, policy updates continue to grapple with these complex issues, aiming to reduce inequalities and promote more equitable access to healthcare and wellness for all populations. The stark reality is that for every extra $1000 spent on healthcare in OECD countries, life expectancy can fall by 0.4 years, indicating that spending alone does not guarantee better health outcomes without addressing underlying systemic issues.
The Spectrum of Care: From Primary Prevention to Specialized Nursing
The healthcare system operates on a multi-tiered spectrum, designed to address varying levels of medical need, from routine check-ups to life-saving interventions. This spectrum typically includes primary, secondary, and tertiary care, each playing a distinct yet interconnected role in maintaining public health.
Primary care serves as the first point of contact for most individuals, focusing on general health, preventive services, and the management of common illnesses. This includes family physicians, general practitioners, and nurse practitioners who provide continuous, comprehensive, and coordinated care. They are crucial for annual wellness visits, routine screenings, and vaccinations, all essential for early detection and prevention of chronic diseases. For instance, annual wellness visits allow for discussions about lifestyle, mental health screenings, and referrals for specialized care, empowering individuals to take charge of their health proactively.
Secondary care involves specialists who focus on specific body systems or conditions, such as cardiologists, dermatologists, or orthopedists. Patients typically access secondary care through a referral from their primary care provider. This level of care is vital for diagnosing and managing more complex conditions that require specialized expertise.
Tertiary care represents highly specialized and complex medical interventions, often provided in large teaching hospitals or regional medical centers. This includes advanced surgical procedures, intensive care, and specialized diagnostics for severe or rare diseases. Facilities like Bozeman Health Deaconess exemplify this, having received a five-star overall hospital quality rating for 2021 from the Centers for Medicare & Medicaid Services (CMS). Bozeman Health, a prominent regional provider, offers a wide range of services from cancer centers to emergency care, supporting the wellness of communities in Southwest Montana.
Chronic disease management is a cornerstone of modern healthcare, especially given that over half of adult Americans live with conditions like heart disease, diabetes, and cancer. Prevention strategies, including lifestyle modifications and regular screenings, are paramount. Annual wellness visits and screenings, such as blood pressure checks, cholesterol tests, and cancer screenings, are essential for early detection and intervention, significantly improving long-term health outcomes. Vaccinations also play a critical role in preventing infectious diseases and maintaining community health.
Specialized nursing, including long-term care and skilled nursing facilities, provides continuous support for individuals who require ongoing medical attention or rehabilitation. These facilities, like those focused on King Street healthcare, are integral for patients recovering from acute illness, managing chronic conditions, or requiring assistance with daily living. Nurses play a crucial role in patient education, medication management, wound care, and emotional support, ensuring a holistic approach to recovery and sustained well-being. This extends to critical care units and Level III trauma centers, where highly skilled nurses are at the forefront of providing life-saving interventions and comprehensive patient management.

Innovations in Fertility and Reproductive Health
The field of fertility and reproductive health has witnessed remarkable advancements, offering hope and solutions to individuals and couples striving to build families. Reproductive endocrinology, a specialized branch of medicine, continues to push the boundaries of understanding and treating infertility.
Innovations in In Vitro Fertilization (IVF) have made the process more refined and successful. Techniques like intracytoplasmic sperm injection (ICSI), preimplantation genetic testing (PGT), and advanced embryo culture systems have significantly improved success rates and reduced the risk of genetic disorders. These advancements allow for more personalized treatment plans, addressing specific challenges faced by patients. Fertility preservation, including egg, sperm, and embryo freezing, has become increasingly vital, offering options for individuals facing cancer treatments, military deployment, or those who wish to delay parenthood for personal or professional reasons.
Maternal health has also seen significant improvements, with a focus on comprehensive prenatal care, advanced fetal diagnostics, and specialized support for high-risk pregnancies. The emphasis is not just on the physical health of the mother and baby but also on their emotional and mental well-being throughout the pregnancy journey. Hormonal balance plays a critical role in reproductive health, and new therapies are continually being developed to address conditions like PCOS, endometriosis, and menopausal symptoms that impact fertility and overall well-being. Organizations like Palmetto IVF healthcare wellness are at the forefront of providing integrated care that combines medical expertise with a holistic approach to reproductive health.
Genetic screening technologies have become more sophisticated, allowing for the identification of genetic conditions in embryos before implantation or early in pregnancy, offering parents more informed choices. Family planning services have also evolved, offering a wider range of contraceptive options and counseling tailored to individual needs and life stages. In 2026, fertility trends indicate a growing interest in personalized reproductive medicine, incorporating lifestyle factors, nutritional guidance, and mental health support alongside traditional medical interventions. This holistic reproductive support acknowledges that conception and pregnancy are deeply intertwined with overall health and wellness.

The Evolution of Aesthetic Medicine and Regenerative Wellness
The landscape of aesthetic medicine has dramatically shifted from purely cosmetic enhancements to a broader focus on regenerative wellness, aiming to restore and optimize the body’s natural functions and appearance from within. This evolution is driven by a deeper understanding of cellular health and the desire for sustainable, long-term well-being.
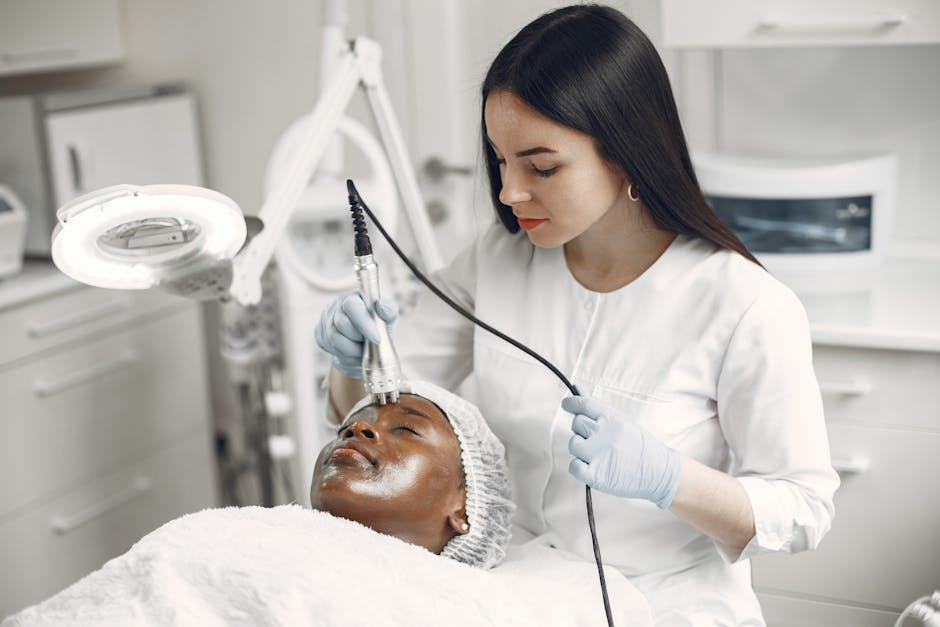
Medical-grade facials and advanced skincare treatments are no longer just about superficial improvements; they are designed to promote skin health at a cellular level, addressing issues like hyperpigmentation, acne, and aging through science-backed ingredients and technologies. Beyond topical solutions, injectable treatments like B12 injections and NAD+ IV therapy are gaining prominence. B12 injections are recognized for their role in combating fatigue, enhancing mood, and supporting overall metabolic function, particularly beneficial for individuals with absorption issues or dietary restrictions. NAD+ IV therapy, on the other hand, targets cellular repair, DNA repair, and energy production. As a coenzyme found in every cell, NAD+ levels decline with age, and replenishing it through IV therapy is believed to contribute to anti-aging effects, improved mental clarity, and enhanced athletic performance. These therapies exemplify the move towards optimizing internal health for external radiance.
The integration of regenerative principles extends to addressing concerns like muscle loss prevention and weight management. New approaches, including the use of GLP-1 medications, are revolutionizing how weight is managed, offering effective solutions for chronic weight conditions by impacting appetite regulation and metabolism. These medical advancements are often complemented by a focus on comprehensive lifestyle changes, including nutrition and fitness, to ensure sustainable results.
The emphasis on Regenerative health and wellness highlights a paradigm shift: treating the root causes of aging and dysfunction rather than just the symptoms. This includes advanced therapies that stimulate the body’s own healing processes, leading to improved skin health, metabolic optimization, and overall vitality. Resources like Healthline: Medical information and health advice you can trust. provide medically-backed guidance on these and many other health topics, helping individuals navigate the complex world of modern wellness. Healthline, with its 19 years of experience and 130 medical reviewers, serves as a trusted source for understanding the science behind these evolving treatments.
Navigating Global Systems and Access
Comparing health systems worldwide reveals a complex tapestry of approaches to healthcare financing, delivery, and outcomes. The United States, for example, stands out with its high healthcare spending, accounting for 18% of its GDP in 2020 and spending $12,555 per capita in 2022 (PPP-adjusted). This contrasts sharply with countries like Canada, which spends $6,319 per capita, or the OECD average. Despite significant investment, the US often lags behind other developed nations in key health metrics like life expectancy and efficiency. In fact, research suggests that in some OECD countries, for every extra $1000 spent on healthcare, life expectancy can paradoxically fall by 0.4 years, indicating that higher spending does not always equate to better health.
Efficiency metrics, such as administrative costs, patient wait times, and health outcomes per dollar spent, vary widely. Many European countries operate under universal healthcare models, often financed through taxes or social insurance, aiming for equitable access. These systems frequently demonstrate better life expectancy and overall population health outcomes, despite lower per capita spending.
Public health initiatives play a crucial role in all systems, focusing on disease prevention, health promotion, and community-wide interventions. These initiatives are often more cost-effective in the long run than treating advanced diseases.
The impact of insurer wellness programs, such as those offered by major providers like Kaiser Permanente, UnitedHealthcare, and Dean Health Plan, is also significant. Kaiser Permanente, named the best health insurance company of 2026 by Insure.com, actively supports patient wellness through integrated care and resources that go “beyond the doctor’s office,” including self-care apps and wellness coaching. Custom Care & Coverage Just For You | Kaiser Permanente highlights their commitment to holistic health. Similarly, Dean Health Plan, a WELCOA platinum award winner, offers comprehensive programs focusing on eight dimensions of wellness, aiming to make healthy living achievable and fun for its members. These programs often include incentives for healthy lifestyles, mental health support, and resources for chronic condition management, contributing to improved workplace productivity and employee retention by fostering a healthier workforce.
Frequently Asked Questions
What is the fundamental difference between healthcare and wellness?
Healthcare typically refers to the organized provision of medical services to treat or prevent illness, focusing on diagnosis, treatment, and recovery from specific health conditions. It’s often reactive, intervening when a problem arises. Wellness, on the other hand, is the active pursuit of activities, choices, and lifestyles that lead to a state of holistic health and optimal well-being. It’s proactive, emphasizing prevention, self-care, and continuous improvement across physical, mental, emotional, social, and other dimensions of life.
Why is preventive care considered essential for long-term health?
Preventive care is essential because it focuses on maintaining health and preventing disease before it starts or progresses. This includes annual wellness visits, regular screenings (e.g., for blood pressure, cholesterol, cancer), and vaccinations. Such measures allow for the early detection of chronic diseases like diabetes and heart disease, which affect over half of adult Americans, significantly improving treatment outcomes and reducing long-term costs associated with advanced disease management. By addressing potential issues early, preventive care helps individuals live healthier, longer, and more fulfilling lives.
How do digital tools assist in modern health management?
Digital tools have revolutionized modern health management by making health information and tracking more accessible and personalized. Apps can provide guided meditations for stress reduction, track sleep patterns, or monitor fitness levels. Symptom checkers offer preliminary guidance based on reported symptoms, while comprehensive health encyclopedias provide medically-backed information on a vast array of conditions. Telehealth platforms enable remote consultations, making healthcare more convenient. These tools empower individuals to monitor their vitals, manage stress, build healthy habits, and access reliable health information, facilitating better self-care and more informed discussions with healthcare providers.
Conclusion
As we look towards the future from April 2026, the convergence of healthcare and wellness marks a pivotal shift towards integrated care models that prioritize the whole person. The extensive guide above underscores that true well-being is a dynamic interplay between reactive medical intervention and proactive lifestyle choices. From the foundational distinctions between healthcare and wellness to the intricate levels of care delivery, and the transformative power of digital tools, every aspect points towards a more empowered and informed individual.
Innovations in specialized fields like fertility and regenerative wellness, alongside the critical role of nursing, are continually expanding the possibilities for healthier lives. Navigating global health systems and leveraging the impact of insurer wellness programs further highlight the collective effort required to foster a healthier society. The future of medicine is undeniably moving towards a model where patient empowerment, preventive strategies, and comprehensive health systems work in concert to achieve sustainable wellness for all.







