The Evolution of Advanced Healthcare Treatments

As of April 2026, we find ourselves in a medical landscape defined by hyper-personalized, technology-driven interventions. Our advanced healthcare treatments now integrate artificial intelligence, robotic precision, and regenerative science to address chronic conditions once considered untreatable. By combining these innovations with robust patient autonomy frameworks, we are not only extending life expectancy but significantly enhancing the quality of life for patients navigating complex urological and pain-related challenges.
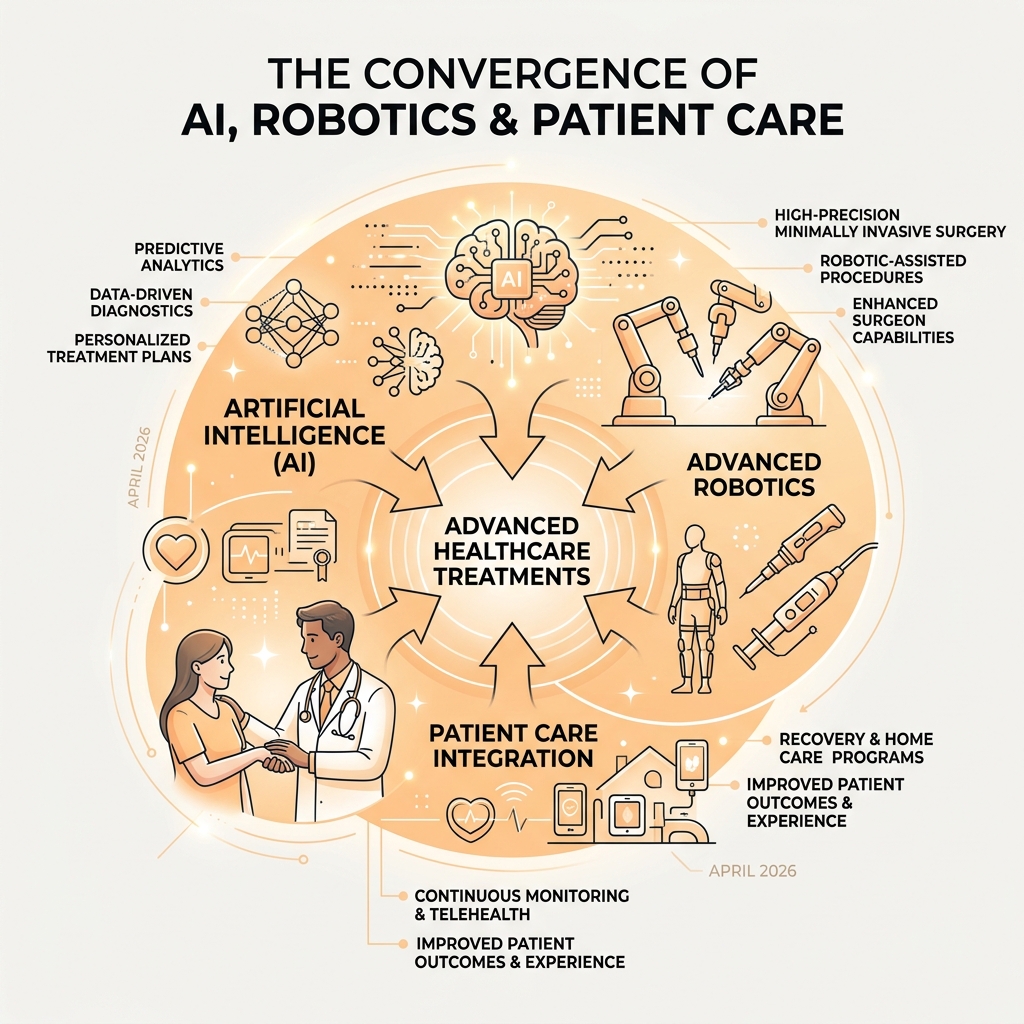

The trajectory of modern medicine is undeniably upward, propelled by a convergence of emerging technologies that are reshaping how we diagnose, treat, and manage health. As healthcare professionals, we observe a profound shift towards patient-centered care, where precision medicine tailors treatments to individual genetic profiles and lifestyle factors. These advancements, particularly prominent in April 2026, are not just theoretical; they are actively improving healthcare accessibility and outcomes across various specialties. For a deeper dive into specialized care, exploring resources on Advanced urology healthcare can provide further context on how these innovations are applied in specific fields.
A prime example of this evolving landscape is the rise of hospital-at-home programs. Pioneered by institutions like the Mayo Clinic, their Advanced Care at Home initiative has successfully treated over 5,500 individuals, demonstrating that high-quality, hospital-level care can be effectively delivered in the comfort and familiarity of a patient’s residence. This model represents a significant step towards making advanced treatments more accessible and less disruptive to daily life.
AI-Driven Diagnostics as Advanced Healthcare Treatments
Artificial intelligence (AI) and machine learning (ML) are no longer futuristic concepts but integral components of our diagnostic toolkit. AI, defined as technology capable of performing complex human tasks, and ML, its branch focused on automating tasks through data processing, are revolutionizing medical diagnostics. These sophisticated algorithms allow for the early and highly accurate detection of diseases, such as various cancers, by meticulously analyzing medical imaging data—often with unprecedented precision that can reduce human error.
The impact of AI extends beyond diagnosis into the realm of drug development. We’ve seen a significant increase in recent years in the number of drug application submissions incorporating AI components, streamlining the research and development process. Furthermore, AI plays a crucial role in predictive analytics, enabling us to forecast health trends and monitor disease outbreaks more effectively. Beyond direct patient care, AI is also proving invaluable in optimizing administrative tasks. For instance, the substantial portion of a nurse’s day—often 30% or more—spent on electronic health record (EHR) documentation can be significantly reduced through AI-powered tools. This optimization of EHRs frees up valuable nursing time, allowing healthcare professionals to dedicate more attention to direct patient interaction and care, addressing the issue of provider burnout. The integration of such technologies is a testament to the ongoing advancements seen in healthcare systems.
Remote Monitoring and Smart Hospitals
The integration of digital technologies has also transformed how we monitor patients and deliver care outside traditional hospital walls. Telehealth, encompassing live video consultations, store-and-forward data transmission, and mobile health (mHealth) applications, has become a cornerstone of modern patient management. Complementing this, remote patient monitoring (RPM) utilizes digital tools to track patient health data in real-time, allowing clinicians to make timely adjustments to treatment plans and intervene proactively.
Wearable health devices are at the forefront of this revolution, evolving from simple fitness trackers to sophisticated medical-grade sensors. These devices, increasingly designed to be discreetly embedded in clothing for enhanced comfort, continuously collect vital health metrics. This real-time data flow is critical for managing chronic diseases, enabling both patients and providers to stay informed and responsive. For example, detailed patient self-reporting, such as Advanced bladder diary instructions, can be seamlessly integrated with remote monitoring platforms, offering a comprehensive view of a patient’s condition.
The concept of “smart hospitals” takes this integration a step further. These facilities leverage interconnected devices and AI to predict patient needs, optimize resource allocation, and enhance overall patient safety. By creating a seamless, data-rich environment, smart hospitals contribute significantly to both real-time patient management and the promotion of preventive care, marking a new era in healthcare delivery.
Breakthroughs in Urology: Minimally Invasive and Robotic Solutions
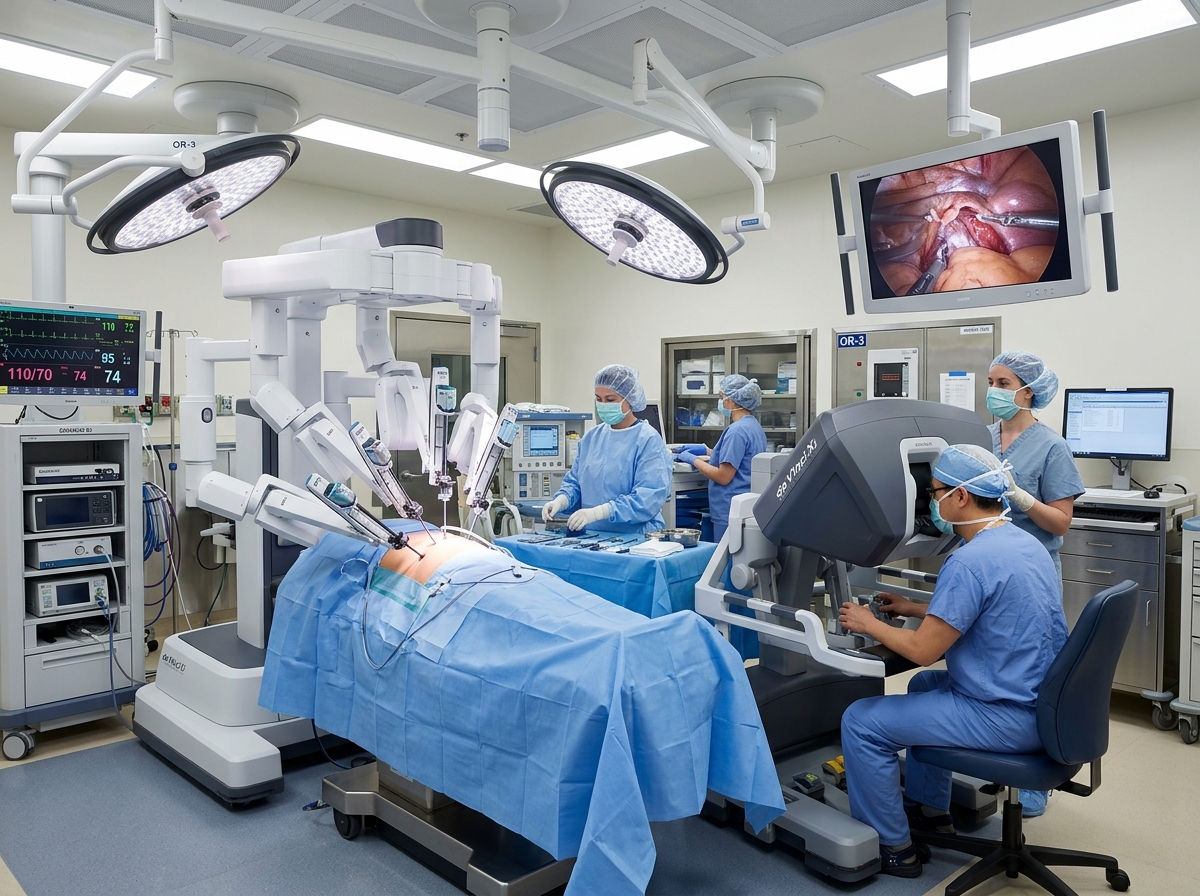
Urology has been a particularly fertile ground for advanced healthcare treatments, with robotic surgery standing out as a transformative innovation. This field has witnessed steady growth, with the robotic-assisted surgery market experiencing a compound annual growth rate (CAGR) of nearly 11%. Robotic surgery enhances a surgeon’s precision, dexterity, and visualization during complex procedures, leading to numerous benefits for patients. These include smaller incisions, reduced blood loss, lower risk of complications, and significantly shorter recovery times. This technology is increasingly vital in sensitive areas such as urologic oncology, where precise tumor removal is paramount.
We utilize robotic systems for a wide array of procedures, including prostatectomies, partial nephrectomies, and bladder reconstructions. Beyond general robotic surgery, specialized technologies like Aquablation Therapy offer a minimally invasive, robotically assisted treatment for benign prostatic hyperplasia (BPH) that uses a heat-free waterjet. Similarly, GreenLight Laser BPH Treatment provides an effective alternative for enlarged prostate, using laser energy to remove excess tissue with minimal invasiveness. These advancements underscore our commitment to providing cutting-edge, less invasive options for our patients.
Advanced Healthcare Treatments for Bladder and Prostate Health
The landscape of treatments for bladder and prostate conditions has been revolutionized by several innovative, minimally invasive approaches. For men suffering from benign prostatic hyperplasia (BPH), Rezum Water Vapor Therapy offers a non-surgical solution that uses steam to reduce excess prostate tissue. This office-based procedure provides lasting relief from urinary symptoms with a quick recovery. Another effective option for BPH is the UroLift System, which involves placing small implants to hold open the prostatic urethra, alleviating obstruction without cutting, heating, or removing prostate tissue. The iTind Procedure provides a temporary implant that reshapes the prostatic urethra to improve urine flow.
For bladder control issues, we have seen significant advancements. Axonics Therapy, a form of sacral neuromodulation, involves implanting a small device that sends mild electrical pulses to the sacral nerves, helping to restore normal bladder function for those with overactive bladder (OAB) or urinary retention. Similarly, Bladder Botox injections can temporarily relax the bladder muscle, reducing symptoms of OAB. To aid in prostate cancer treatment, SpaceOAR Hydrogel is an innovative solution that creates space between the prostate and rectum during radiation therapy, significantly reducing radiation exposure to healthy tissue and minimizing side effects. These treatments collectively represent a paradigm shift towards more targeted, less invasive, and highly effective care for common urological conditions, improving patient outcomes and quality of life.
Innovations in Pelvic Health and Reconstruction
Beyond treating specific conditions, modern urology is making strides in overall pelvic health and reconstructive procedures. The EMSella Chair offers a groundbreaking, non-invasive therapy for urinary incontinence and pelvic floor weakness. Patients simply sit on the chair fully clothed, and electromagnetic technology stimulates the pelvic floor muscles, leading to significant improvements in muscle strength and bladder control. This approach to pelvic floor rehabilitation is transforming how we address these common, yet often debilitating, issues.
Our commitment to comprehensive patient care extends to complex reconstructive urology, where advanced diagnostic tools and surgical techniques are used to repair and restore function to the urinary and reproductive systems. These efforts are crucial for improving the quality of life for individuals with congenital anomalies, trauma, or cancer-related damage. Specialized healthcare systems are increasingly integrating these sophisticated diagnostic capabilities to ensure thorough evaluation and personalized treatment plans. As part of a holistic approach to patient well-being, many centers now offer a broad spectrum of services, encompassing not only surgical interventions but also supportive therapies aimed at optimizing recovery and long-term health.
Advanced Pain Management and Regenerative Therapies
The intersection of advanced pain management and regenerative therapies marks a new frontier in healthcare, offering hope for conditions previously deemed untreatable. Chronic pain, often complex and debilitating, is now being approached with innovative strategies that move beyond symptomatic relief to address the underlying causes. For individuals seeking comprehensive solutions, exploring Advanced pain management treatments can reveal a range of options from interventional procedures to cutting-edge biologics.
Regenerative medicine, in particular, is an exciting area. It encompasses stem cell therapy, tissue engineering, and gene therapy, aiming to restore or regenerate damaged tissues and organs. Alongside this, groundbreaking immunotherapies like CAR T-Cell Therapy are revolutionizing cancer treatment by genetically engineering a patient’s own immune cells to target and destroy cancer. The rapid development and adaptability of mRNA vaccines, initially highlighted during the COVID-19 pandemic with reported efficacy rates of 95% for Pfizer-BioNTech and 94.1% for Moderna, continue to evolve for other diseases, including influenza, HIV, and even certain cancers. This adaptability underscores their potential for rapid response to new health threats and personalized medicine. Targeted drug delivery, often facilitated by nanotechnology, further enhances treatment efficacy by precisely delivering therapeutic agents to affected cells, minimizing systemic side effects.
Regenerative Medicine: The Future of Advanced Healthcare Treatments
Regenerative medicine is rapidly emerging as a cornerstone of advanced healthcare treatments, offering unprecedented possibilities for healing and recovery. Nanotechnology plays a pivotal role here, enabling targeted drug delivery directly to diseased cells, and even the development of nanobots designed to detect and destroy cancer cells within the body. CRISPR gene editing, a tool, allows for precise modifications to DNA, opening doors for treating genetic disorders. We’ve already seen promising results, such as an infant treated with personalized CRISPR therapy for a genetic deficiency who is now thriving.
The realm of implantable artificial organs is also expanding, driven by innovations like 3D bioprinting. This technology is advancing rapidly, with researchers working towards creating functional lab-grown organs and tissues for transplantation, moving beyond customized prosthetics and implants. The goal is to develop artificial organs that mimic natural organ shape and functionality, using advanced polymers or biological tissues. This field also holds immense promise for nerve regeneration, offering new hope for individuals with spinal cord injuries or other neurological damage. Many specialized healthcare services are at the forefront of developing and delivering these personalized biologics, tailoring treatments to each patient’s unique biological makeup for optimal outcomes.
Neuromodulation and Non-Pharmacological Pain Relief
In the pursuit of comprehensive pain management, neuromodulation techniques and non-pharmacological therapies are gaining prominence, particularly in reducing reliance on opioids. Virtual Reality (VR) therapy, for instance, is increasingly used for non-pharmacological pain relief during procedures or for chronic pain conditions, distracting patients and altering pain perception. More invasive but highly effective options include deep brain stimulation and spinal cord stimulation, which involve implanting devices to deliver electrical impulses that block pain signals or modulate brain activity.
Biofeedback, a non-invasive technique, teaches patients to control involuntary bodily functions like heart rate and muscle tension, empowering them to manage their pain responses. These approaches are often integrated into holistic treatment plans offered by advanced hospital and clinic networks, emphasizing a multidisciplinary strategy for pain relief. By combining these innovative therapies, we can provide effective pain management while significantly reducing the risks associated with long-term opioid use, ultimately improving patients’ quality of life.
The Role of Patient Autonomy and Advance Care Planning
Amidst the rapid advancements in medical technology, the fundamental importance of patient autonomy remains paramount. Advanced care planning (ACP) is a critical component of this, empowering individuals to make informed decisions about their future medical care, especially if they become seriously ill or unable to communicate. This process involves not only conversations with loved ones and healthcare providers but also the creation of legal documents known as advance directives. These directives typically include living wills, which outline specific medical treatments a person wishes to accept or refuse, and durable power of attorney for health care, designating a trusted individual (a healthcare proxy) to make decisions on their behalf.
The necessity of clear advance directives is underscored by a sobering statistic: in one study, loved ones guessed nearly one out of three end-of-life decisions for their family members incorrectly. This highlights the profound need for explicit planning to ensure a patient’s wishes are honored and to alleviate the immense burden on family members during difficult times. Patient advocacy is central to this process, ensuring that an individual’s values and preferences guide their care. Ethical considerations are deeply intertwined with these discussions, particularly as advanced treatments offer increasingly complex choices. While specific guides are invaluable resources for this process, the core principle remains open communication and proactive planning to safeguard patient autonomy.
Navigating Challenges in High-Tech Healthcare
While advanced healthcare treatments promise remarkable benefits, their rapid integration also presents significant challenges that require careful navigation. Cybersecurity is a paramount concern, as the increasing digitalization of patient data makes healthcare systems attractive targets for malicious attacks. Robust measures are essential to protect sensitive health information from breaches. Closely related is data privacy, ensuring that patient data is collected, stored, and used in compliance with regulations like HIPAA.
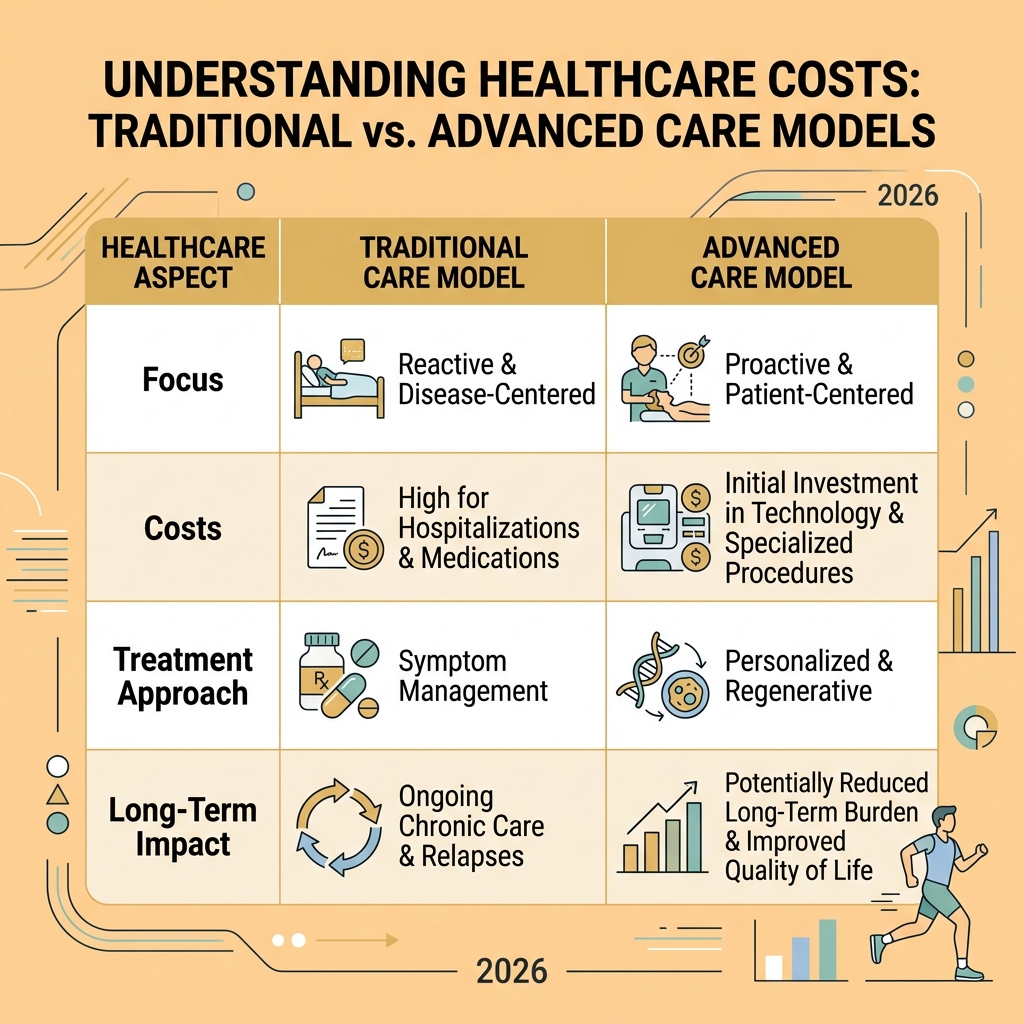
Blockchain technology is emerging as a potential solution to enhance data security and integrity. By creating decentralized, immutable records, blockchain can ensure HIPAA-compliant data security, making patient records tamper-proof and auditable. However, the adoption of such innovative solutions often faces regulatory hurdles, as existing frameworks may not fully address the complexities of new technologies. Ethical AI use is another critical area, requiring careful consideration of algorithmic bias, transparency, and accountability in clinical decision-making. Finally, the cost-effectiveness of these advanced treatments is a constant challenge. While many innovations offer superior outcomes, their high price tags can create accessibility barriers, particularly for patients in rural areas or those with limited insurance coverage. Addressing these challenges requires collaborative efforts from policymakers, healthcare providers, technologists, and patients to ensure equitable access and responsible implementation.
Frequently Asked Questions about Advanced Healthcare
What are the most prominent emerging healthcare technologies in 2026?
As of April 2026, the healthcare landscape is being reshaped by several prominent emerging technologies. These include:
- AI Diagnostics: Revolutionizing early disease detection and medical imaging analysis.
- Robotic-assisted Surgery: Enhancing precision and minimally invasive procedures across various specialties, particularly in urology.
- CRISPR Gene Editing: Offering groundbreaking potential for treating genetic disorders and certain cancers.
- mRNA Vaccines: Expanding beyond infectious diseases to target cancers and other conditions with rapid adaptability.
- Wearable Health Monitors: Providing real-time patient data for chronic disease management and preventive care.
These innovations collectively represent a significant leap forward in personalized and effective patient care.
How do advance directives protect patient autonomy?
Advance directives are crucial legal documents that safeguard a patient’s autonomy by formally expressing their wishes regarding medical treatment. These include living wills, which detail specific interventions a person wants or doesn’t want, and durable power of attorney for health care, which designates a trusted individual to make medical decisions if the patient is unable to communicate. By establishing these directives, patients ensure their end-of-life wishes are respected, even when incapacitated. This proactive planning reduces the emotional burden on family members, prevents potential disagreements, and ensures that care aligns with the patient’s values and preferences.
What is the role of hospital-at-home programs?
Hospital-at-home programs represent a significant evolution in healthcare delivery, providing hospital-level care to eligible patients in their own homes. These programs leverage remote patient monitoring (RPM) and virtual care teams to deliver comprehensive medical services, including IV therapy, mobile imaging, and daily virtual visits. The role of these programs is multifaceted: they enhance patient comfort and satisfaction, reduce the risk of hospital-acquired infections, and can lead to lower readmission rates. For example, the Mayo Clinic’s Advanced Care at Home program has demonstrated successful outcomes for thousands of patients, proving that high-quality, acute care can be effectively and safely managed outside traditional inpatient settings.
Conclusion
The landscape of advanced healthcare treatments in 2026 is a testament to human ingenuity and the relentless pursuit of better patient outcomes. From the precision of robotic urologic surgery to the life-altering potential of CAR T-cell therapy and regenerative medicine, these innovations are redefining the boundaries of what is possible. However, the true success of these technologies lies in their integration with compassionate care and robust advance care planning. As we continue to adapt to these rapid changes, the focus remains clear: empowering patients through technology while safeguarding their autonomy and dignity.
Author Bio: Dr. Lawrence Reed, MD, is a board-certified specialist in clinical innovation with over 20 years of experience. He focuses on integrating emerging technologies into patient-centered care models to improve long-term health outcomes.







