By Phillip Miller
The prognosis for rural hospitals is not a positive one. According to the North Carolina Rural Health Research Program, 90 rural hospitals have closed nationwide since 2010. A 2015 study sponsored by the National Rural Health Association (NRHA) indicates that 673 rural hospitals, or one in three, is under financial duress, with 210 at risk of closure.
There are various reasons why rural hospitals are struggling, a key one being lack of physicians willing to practice in rural areas. The NRHA reports that approximately 1,000 physicians a year discontinue rural practice due to retirement, relocation, disability or death, while only about 700 take their place.
The result is that access to medical services in rural areas continues to decline. As of July, 2018 there were 6,739 Health Care Professional Shortage Areas (HPSAs) for primary care in the United States, about double the number identified by the Health Resources and Services Administration (HRSA) 15 years ago. Over 65 million people live in a primary care HPSA and 67 percent of HPSAs are in rural areas. The ratio of primary care providers to patients in these areas is less than one per 3,000. HRSA projects it would take over 17,000 additional primary care clinicians to achieve a ratio of one primary care doctor per 3,000 patients in the nation’s 6,700-plus HPSAs.
HRSA also currently designates approximately 4,931 mental health HPSAs nationwide in which over 80 million Americans live. These are areas in which there is less than one psychiatrist per 30,000 people. Rural areas in particular struggle to maintain psychiatric services. Texas, a large rural state, has 185 counties with no psychiatrist according to the Merritt Hawkins study: The Physician Workforce in Texas.
Physicians are essential to providing their communities with needed healthcare services, but they also play a vital economic role for their hospitals. According to Merritt Hawkins 2019 Physician Inpatient/Outpatient Revenue Survey , physicians on average generate an average of $2.38 million a year for the hospitals with which they are affiliated. In the case of rural physicians, this number can be much higher. Without physicians to admit patients, order tests and perform procedures, hospitals lack the revenue they need to stay open. When rural hospitals close, the communities they serve typically lose both their largest employer and their prospects for future economic development and growth.
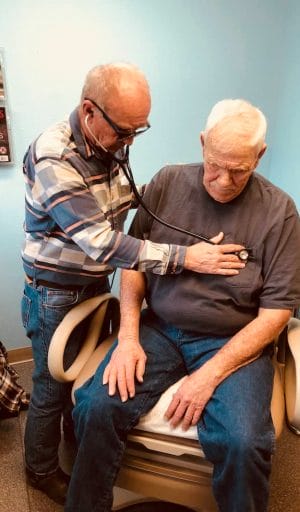
This common pattern could well have played out in tiny Bieber, California if not for the continued presence of Dr. Daniel Dahle, recently named the 2019 Country Doctor of the Year by Staff Care, a national physician staffing firm.
Serving an area larger than five states and a community 45 miles from the nearest traffic light, Dr. Daniel Dahle is the medical version of a hero in a Clint Eastwood western, keeping the local citizens safe not with six shooters but with over three decades of medical expertise and an unflinching commitment to personalized care.
While seeing patients at Big Valley Health Center in Bieber, Dr. Dahle also drives 25 miles one way almost every day to see inpatients at Mayers Memorial Hospital in Fall River Mills, where he also covers the emergency department and cares for long-term patients at the hospital’s nursing home. Over half the hospital’s inpatients are admitted by Dr. Dahle, and his presence in the community has been vital to the hospital’s continued viability.
Now aged 70 and contemplating retirement, Dr. Dahle has made educating future care givers part of his mission. Each year he provides training to medical residents from the University of California, Davis as well as students from the physician assistant program at the University of Iowa. Dr. Dahle is hoping to pass the torch on to a husband and wife duo who will soon be completing their medical training and who Dr. Dahle has been recruiting since the couple was in medical school, but the situation remains fluid.
That would go a long way to solving one community’s dilemma, but what is really needed is a broader national effort to increase physician supply in rural areas. This could include lifting the cap on federal funding of physician graduate medical education imposed by Congress in 1997, expanding rural residency programs, more scholarships for rural students contemplating going into medicine, and a greater sense of urgency about this problem.
Meanwhile, the citizens of Bieber and a vast surrounding area of 7,500 square miles from which Dr. Dahle draws patients, hope he will postpone his exit from medicine and continue to be their physician. A lot is riding on his continued presence in the community, and the continued presence of thousands of country doctors in similar places nationwide.
Phillip Miller is Vice President of Communications for Staff Care and Merritt Hawkins, companies of AMN Healthcare, the nation’s leading provider of healthcare staffing solutions.
Throughout the year, our writers feature fresh, in-depth, and relevant information for our audience of 40,000+ healthcare leaders and professionals. As a healthcare business publication, we cover and cherish our relationship with the entire health care industry including administrators, nurses, physicians, physical therapists, pharmacists, and more. We cover a broad spectrum from hospitals to medical offices to outpatient services to eye surgery centers to university settings. We focus on rehabilitation, nursing homes, home care, hospice as well as men’s health, women’s heath, and pediatrics.







