By Stacey Lang, RNC, BSN, CNRN
Senior VP, Corazon, Inc.
Much has been written about the rapidly changing healthcare landscape, though perhaps reimbursement trends are what’s keeping even the savviest of healthcare leaders awake at night. Value over volume, quality over quantity, full continuum disease episode accountability, and the ever-present and increasing patient experience and satisfaction expectations all require a renewed focus, along with a consistent and seamless approach to care delivery.
Corazon believes – whether in cardiovascular, neuroscience, or orthopedics – that expanding treatment options across each of these service lines brings great potential for improved patient outcomes. Not coincidentally, these three services are most often associated with high costs-per-case and shrinking margins. But indeed, the ability to positively impact not only patient outcomes, but also program finances, does exist, particularly when proven therapies are administered through a process- and protocol-driven approach.
As the complexity of treatments increases, so does the importance of a strong and dedicated focus on care delivery. In an effort to further drive a broad quality improvement effort, states, payors, and even pre-hospital providers often require an additional level of scrutiny through a formal accreditation or certification process before patients can be treated.
Corazon has both national experience and a proven reputation in preparing organizations for certification and/or accreditation, and also in serving as the accrediting body in several states, including Pennsylvania and Michigan. Our exposure to organizations all over the country has served to illustrate three distinct advantages for those that take the necessary steps to achieve program accreditation and/or certification:
- Increased volume capture
- Decreased costs and improved margins
- Enhanced quality
The following examples illustrate some benefits of accreditation realized by many of our clients within the aforementioned key service lines. The achievements described for the service lines in these case studies can certainly be realized through accreditation for ANY clinical service, however. These examples can serve as a guide for others considering accreditation as a means to show what types of positive changes can be realized through this valuable effort.
Stroke
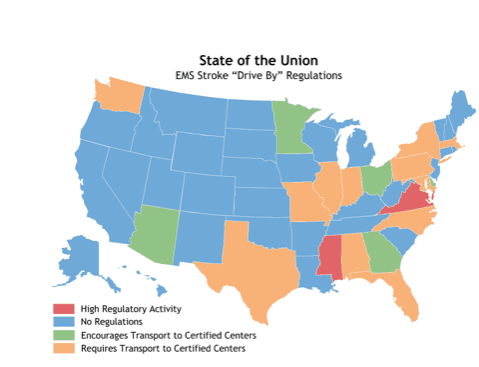
There is perhaps no greater example of the role that formal certification can play in expanded volume capture than in the case of stroke care. In fact, many states require formal certification as a stroke program (Primary, Comprehensive, or Stroke-Ready) in order for EMS providers to transport suspected stroke patients to the facility. We’ve seen the number of states adopting this approach increase significantly over the past several years, likely because without the risk of needing transfer for care, ptients are faring better at their first stop for treatment.
The map below identifies those states with established transport protocols in place, as well as those where changes were anticipated as of December 2014.
FIG 1:
While tremendous strides have been made in available treatments for patients affected by stroke, challenges continue to exist in delivering that care within the required time parameters. Administration of thrombolytics remains the best first-line treatment for stroke. But, despite the clear benefit, treatment percentages range from only 7% to 30% nationally. In other words, only 7% to 30% of patients who are eligible to receive this treatment actually do. Providing care that is protocol- and process-driven has been proven to significantly increase these percentages.
Technology can be used as one way to implement protocols and processes that drive consistent care models so that patients receive the same care 24/7/365 – the right care is given to the right patient at the right time. Corazon’s Cerebros system is a proven solution for reaching this goal. As one of only four finalists in “The Challenge” at the 2016 Cleveland Clinic Innovations Summit, the system’s demonstrated benefits stood-out among approximately 100 entrants for the best new technology to change how patients receive care.
Though the requirements for achievement of certification for a stroke program are rigorous, the process of program development fosters a culture of process-driven multi-disciplinary care that often positively impacts patients beyond those being treated only for stroke. Further, national experience demonstrates that successful stroke program certification enhances relationships with EMS providers by increasing confidence in the ability to provide emergent care to high-acuity patients in a consistent way. Given the parameters under which EMS functions, any patient who presents with symptoms that “may be consistent with stroke” must be transported to a designated stroke (or in some cases, stroke-ready) center. This mandate significantly expands the pool of patients who would be transported for treatment. This increased volume, combined with a high degree of efficiency in care delivery yields greater margins through decreased costs and length of stay, along with enhanced quality and consistency of care.
Orthopedics
Management of implant costs has long been an area of focus in organizations that have the benefit of a busy orthopedic program. A singular focus in this area has become less impactful over time as device manufacturers have worked to reduce costs as a result of broad-based industry pressure. New challenges related to bundled payments, physician employment and alignment, and vendor loyalty serve to significantly complicate the management of this service. And no doubt these challenges will remain in place for the years to come.
Those organizations that commit to achieving accreditation as a Total Joint Program of distinction are, in many ways, forced to jump-start much of the difficult work in aligning physician and hospital goals, establishing a collaborative vendor-selection process, and adopting uniform processes that result in exceptional patient outcomes and satisfaction. These goals would benefit any program, so achieving them along with the added accreditation certainly has the potential to catapult a program beyond the status quo.
Achieving consensus from all involved in full-continuum care with respect to treatment algorithms and protocols, patient selection, rehabilitation needs, and LOS expectations are mandated requirements associated with accreditation. And, these same steps are key foundational elements of preparedness for the new reimbursement paradigm of bundled payments – a win-win result from one effort bringing dual benefits. Further, the decrease in costs from this unified vision can lead to enhanced profitability; and, in some cases, financial viability can be all but assured for orthopedic programs of distinction.
Cardiovascular Services
Some of the early steps in implementing protocol-driven care occurred in the area of cardiovascular services. Initially, Percutaneous Coronary Intervention (PCI) could only be performed in hospitals with on-site open heart surgery (OHS) capabilities. More recently, PCI with off-site surgical support became permitted in some states, but not without a very rigid set of requirements. Now, several states, including Pennsylvania, Michigan, and California, are requiring accreditation or verification by an outside agency to demonstrate compliance with the many regulations that accompany this expansion of services.
In addition to well-defined protocols, treatment pathways, and educational and training requirements, organizations must collect and submit data via the ACC-NCDR database in order to be granted permission to offer PCI with off-site OHS. This provides an ongoing opportunity for individual facility quality reviews, as well as benchmarking against ‘like’ organizations at a national level. Quality outliers are quickly identified, and a demonstrated plan of corrective action is required to maintain accreditation. The data collection also aids in tracking Appropriate Use Criteria (AUC) results, a major area of focus for any cardiovascular program.
Collated national data gathered from the time since PCI with off-site surgical support has been permitted demonstrates that these procedures can and are performed safely and to the patient’s benefit when the established criteria are followed. In fact, Corazon client experience with dozens of these engagements proves that the enhanced quality of care delivery that results from achieving the goals of accreditation most certainly leads to optimal treatment for cardiac patients.
While the path to accreditation or certification can be challenging, the demonstrated benefits far outweigh the financial and manpower investment of the effort. Given the rapidly-evolving healthcare reimbursement landscape, the question is no longer “if” formal certification of clinical programs will be required, but rather “when.” Forward-thinking organizations are embracing these changes and moving to incorporate accreditation into programming plans for the short-term future…. The sooner the initiative is launched, the sooner improvements will be realized on behalf of the clinical / operational / and financial aspects of the organization, along with the individual patients served within a community. There are fewer accolades that better communicate a program’s worth than formal accreditation and the resulting benefits – the time is now to consider this strategy…your patients (AND program stakeholders at all levels) will thank you!
Corazon offers consulting, recruitment, interim management, and information technology services to hospitals and practices in the heart, vascular, neuro, and orthopedics specialties. Find Corazon on facebook at www.facebook.com/corazoninc or on LinkedIn at www.linkedin.com/company/corazon-inc. To learn more about Corazon’s accreditation or other services, or to schedule a free demo of Corazon’s Cerebros Neuroscience software, call 412-364-8200 or visit www.corazoninc.com. To reach the author, email [email protected].
Throughout the year, our writers feature fresh, in-depth, and relevant information for our audience of 40,000+ healthcare leaders and professionals. As a healthcare business publication, we cover and cherish our relationship with the entire health care industry including administrators, nurses, physicians, physical therapists, pharmacists, and more. We cover a broad spectrum from hospitals to medical offices to outpatient services to eye surgery centers to university settings. We focus on rehabilitation, nursing homes, home care, hospice as well as men’s health, women’s heath, and pediatrics.